In our last blog post, we explored the timeline of diagnostic imaging and radiotherapy developed using x-rays. It was the original discovery of x-rays by Röntgen that led to the creation of these medical practices. However, other researchers of the 20th century also invented diagnostic tools and radiation therapy without x-ray involvement at all. We will explore a few of these imaging and radiotherapy machines or procedures in this blog.
Diagnostic Imaging
MRI
One of the most well-known imaging procedures is MRI, which stands for Magnetic Resonance Imaging. Research for MRI began early in the 1970s, but investigation of the magnetic resonance principles started as early as 1945. By happenstance, Felix Bloch, a Swiss physicist working at Stanford, and American physicist, Edward Mills Purcell at Harvard, conducted—nearly simultaneously—an experiment for a new mode of nuclear induction. This led to published papers from both physicists on nuclear magnetic resonance. After publication, both Purcell and Bloch won the 1952 Nobel Prize for this research.1
The process to produce 2D images in an MRI using nuclear magnetic resonance (NMR) was discovered by Paul Lauterbur and Peter Mansfield. Lauterbur published the first nuclear magnetic image in 1973, eventually producing 3D images as well. However, he still had long to go before these images would be practical for application with actual patients. Mansfield continued to expand on Lauterbur’s work, developing the echo-planar imaging technique to improve image quality and scan time in the late 1970s. By 1977, physician Raymond Damadian created the first full body MRI machine. Through continuous improvements and further research, today’s MRI provides a safe, effective way of capturing images in the brain, portions of the body, the cardiovascular system, and central nervous system. MRIs provide information on size, location, classification, and grade of lesions so as to aid diagnosing stroke, MS, blood supply issues, and any brain damage.2
Ultrasound
Today, ultrasound is most widely known in the OB/GYN field of medicine. Through its invention, however, this diagnostic tool proved its range of utility before becoming a staple in wellness checks during pregnancies. The origin of ultrasonography is often credited to Lazzaro Spallananzi, a physiologist who discovered echolocation throughout 1794 from various experiments involving bats. The principles that serve as a basis for echolocation are also those functioning for medical ultrasound technology today. In 1942, neurologist Karl Dussik first used ultrasonic waves in a diagnostic procedure while attempting to find brain tumors. He later published a report of musculoskeletal ultrasonography in 1958, laying the groundwork for diagnostic musculoskeletal ultrasound.3
Professor Ian Donald from the University of Glasgow was responsible for the development of medical ultrasound in clinical practice. During his research from the late 1950s into the 1960s, there was clinical skepticism about the use of ultrasound. Many doctors felt that manual abdominal and pelvic examinations had proven adequate for medical diagnoses. With his co-workers, Donald performed several studies to show the likelihood of misdiagnoses of a cyst versus a malignant mass. By publishing the findings in 1958, this became a critical point in time for encouraging use of the medical ultrasound. Donald and his colleagues eventually developed an automatic scanner that utilized a full bladder for early pregnancy detection in 1963. This set the path to the now common practice of ultrasounds in the OB/GYN field today.4
PET Scans
Experimental physicist, C.D. Anderson, observed particles from cosmic rays in 1932 that were the same mass as an electron, but which moved in a strong magnetic field along a path opposite to that of an electron indicating a positive charge. He named these particles as “positrons” or positive electrons.
Emission of these positrons was the proof that Irène Joliot-Curie and Frédéric Joliot-Curie used to prove the artificial creation of radioactive elements to win the 1935 Nobel Prize in Chemistry. The creation of these artificial elements was the main focus over the following years due to their significance to military research from the late 1930s until the 1950s. Imaging studies began taking strides as a result of the desire by Louis Sokoloff, an American neuroscientist who hoped to relate mental function to brain function. This encouraged research through the 1950s until the first tomography unit attempt in 1968. This was the turning point in which PET scan development accelerated into the machines we are more familiar with today.5
PET scans can provide imaging through the detection of the gamma ray pairs that are created when a positron annihilates with an electron inside the tissue where the positron emitting isotope has collected. Whereas other diagnostic scans capture the form of an object, PET scans correlate with the metabolic functions of the tissues that uptake the radioactive compound. The compound with the radioactive tracer is typically a form of glucose called FDG (fluorodeoxyglucose), which is used as an energy source by cells and is given to the patient by means of an IV injection. The more rapid the metabolism of the cells in a tissue, as you have with cancer cells, the more uptake of the FDG. This differential uptake is then seen as an enhanced region on a PET scan. 5
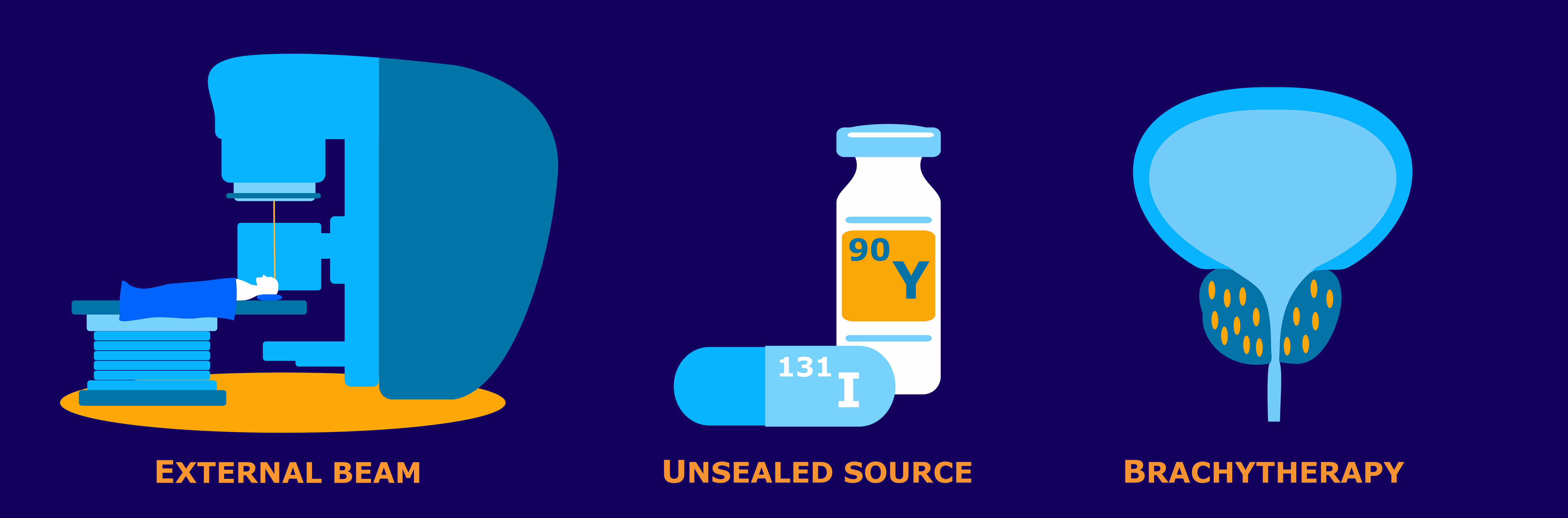
Radiation Therapy
Gamma Rays – Gamma Knife (and Cobalt Therapy)
Gamma radiation from radioactive cobalt sources has been harnessed to create an alternative method for producing therapeutic radiation beams. Similar in design to the previously discussed LINAC machines, a Cobalt unit uses a single Co-60 source to produce the radiation beam for treatment. A machine of a fundamentally different design, the Gamma Knife was developed for the treatment of brain tumors. The Gamma Knife is a stereotactic radiosurgery technique that allows for functional neurological surgery. This machine uses anywhere from 192 to 201 C0-60 arrayed in a semi-spherical shield with each source collimated to point their radiation to the same point in space. This type of precision allows for the potential to treat brain tumors and, in turn, pain, movement disorders, and even some behavioral disorders for patients who had not been responsive to other treatment.6
The Gamma Knife was created through the inspirations of Swedish professors Borje Larsson and Larks Leksell in the 1950s. After an investigation using proton beams with stereotactic devices capable of pinpointing targets in the brain, the researchers eventually gave up on that approach due to cost and complexity. Motivated to find an alternative, Larsson and Leksell went on to create a prototype Gamma Knife system in 1967. The prototype unit was a success, used in Sweden for twelve years and led to a second Gamma Knife in 1975, before other units began appearing globally in the 1980s.6
Proton Therapy
Protons were discovered in the early 1900s. New Zealand physicist Ernest Rutherford’s research during this time led to his discovery of a nuclear reaction that led to the “splitting” of an atom, where he found protons. As a charged particle, the protons have a finite range in matter. The proton’s interaction with matter produces ionization as the proton slows down along its path, losing energy. A peak of deposited dose then occurs at a depth that is proportional to the proton’s original energy.7
The cyclotron, invented by the American physicist Ernest O. Lawrence along with his associates in 1929, proved an efficient way to produce beams of protons. The cyclotron was capable of accelerating protons to high enough energy that, towards the middle of the 20th century, it was suitable for application in cancer treatments.
Dr. Robert Wilson, another American physicist, was the one to spark the idea of proton therapy for battling cancer. He wrote a seminal paper on the functionality of particle beams (comprised of either protons or other heavy-charged particles) and their ability to disperse their energy in the body—the initial release would be small, then exponentially grow when the beam reaches the end of its path for maximum effect against the tumor. Dr. Wilson published the paper in 1946 and received credit to being the inspiration of further research on proton therapy and the continued development of cyclotrons.7
Brachytherapy and Interstitial Therapy
Brachytherapy is an internal radiation therapy technique involving direct placement of radiation inside a patient’s body cavity. This procedure involves small, radioactive source implants that are generally positioned in a body cavity to be near a cancerous tumor. The radioactive material, typically encapsulated within suitable housing material such as titanium, constantly exposes the tumor to a stream of radiation until removal of the radioactivity. These implants will be temporary, and the patient is either hospitalized or kept in a special suite for the duration of the treatment.
Another form of therapy, interstitial therapy (or interstitial brachytherapy), uses sources that are placed directly into the tissue. These may either be temporary or permanent implants of small, encapsulated sources on the order of the size of a rice grain. For treatments with permanent implants, it is safe enough for the patient to go home with a few simple safety guidelines to follow.8
Brachytherapy was first used in 1901 during an attempt to treat lupus. Alexandre Danlos and Paul Bloch completed this treatment with a radioactive sample from Marie Curie. Shortly after, in 1903, Margareth Cleaves used brachytherapy to treat cervical cancer. It became a popular radiotherapy technique to treat breast, cervical, and prostate cancer. As technology advanced along with the use of brachytherapy through the 1900s, imaging-guidance became a valuable asset. More precise dosimetry became possible and allowed for better brachytherapy planning when doctors could use diagnostic modalities such as CTs, MRIs, or ultrasounds. Today, brachytherapy is a more popular treatment for conditions ranging through gynecological, genitourinary, ocular, and head & neck cancers.9
Summary and Conclusion
The 20th century saw tremendous growth and development in diagnostic machinery and radiotherapy. From soundwave technology that gave way to ultrasound, magnetic resonance inspiring MRIs, and the discovery of positrons, medical and non-medical fields can run diagnostic imaging that suits their needs exactly for the most effective information. Radiation therapy research continuously improves the technology and practices used for the wellbeing of patients. Precision instruments such as the Gamma Knife, Cyberknife, and modern LINACs permit for types of treatments that would otherwise be impossible whilst at the same time reducing the side effects associated with external beam therapy. Proton therapy calculations allow for precise travel through the body for maximum effect against cancerous tumors. Brachytherapy provides a treatment option that directly targets tumors without having radiation travel through the body to the target tissue. Modern image guidance ensures source placement exactly where treatment is necessary and that externally directed therapy beams hit their target. As these modalities evolve, we witness the growing reality of safer, more effective diagnoses and cancer treatments within our lifetimes.
The Versant Physics team has experience that covers a range of equipment. This includes dental units, mobile c-arms and Cone-beam CTs, as well as high energy LINACs and even Proton Therapy units and Cyclotrons. To learn more about how our services can help you, contact us to set up a meeting.
Sources
1. NMR Basics | Nuclear Magnetic Resonance Spectroscopy Facility | University of Colorado Boulder. www.colorado.edu. https://www.colorado.edu/lab/nmr/nmr-basics
2. The History of the MRI – DirectMed Parts & Service. https://directmedparts.com/history-of-the-mri/
3. D. Kane and others, A brief history of musculoskeletal ultrasound: ‘From bats and ships to babies and hips’, Rheumatology, Volume 43, Issue 7, July 2004, Pages 931–933, https://doi.org/10.1093/rheumatology/keh004
4. History of Ultrasound – Overview of Sonography History and Discovery. Ultrasoundschoolsinfo.com. Published December 27, 2021. https://www.ultrasoundschoolsinfo.com/history/
5. Henry N. Wagner, A brief history of positron emission tomography (PET), Seminars in Nuclear Medicine, Volume 28, Issue 3, 1998, Pages 213-220, ISSN 0001-2998, https://doi.org/10.1016/S0001-2998(98)80027-
6. History and Technical Overview | Neurosurgery. Neurosurgery. Published 2018. https://med.virginia.edu/neurosurgery/services/gamma-knife/for-physicians/history-and-technical-overview/
7. History of Proton Therapy – NAPT. NAPT. Published 2018. https://www.proton-therapy.org/about/history-of-proton-therapy/
8. Radiation Oncology. Radiation Answers. Accessed May 31, 2023. https://www.radiationanswers.org/radiation-sources-uses/medical-uses/radiation-oncology.html
9. Mayer C, Kumar A. Brachytherapy. PubMed. Published 2021. https://www.ncbi.nlm.nih.gov/books/NBK562190/